Journal Description
European Burn Journal
European Burn Journal
(formerly European Journal of Burn Care) is an international, peer-reviewed, open access journal on burn care and burn prevention. The journal is owned by the European Burns Association (EBA) and is published quarterly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within ESCI (Web of Science), and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 24.7 days after submission; acceptance to publication is undertaken in 5.6 days (median values for papers published in this journal in the first half of 2024).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
- Companion journal: Healthcare.
Impact Factor:
1.0 (2023);
5-Year Impact Factor:
1.0 (2023)
Latest Articles
Qualitative Descriptive Research Investigating Burn Survivors’ Perspectives on Quality of Care Aspects
Eur. Burn J. 2024, 5(3), 215-227; https://doi.org/10.3390/ebj5030021 (registering DOI) - 1 Jul 2024
Abstract
Burn care quality indicators are used to monitor and improve quality of care and for benchmark purposes. The perspectives of burn survivors, however, are not included in current sets of quality indicators while patient-centred care gains importance. The aim of this study was
[...] Read more.
Burn care quality indicators are used to monitor and improve quality of care and for benchmark purposes. The perspectives of burn survivors, however, are not included in current sets of quality indicators while patient-centred care gains importance. The aim of this study was to explore burn survivors’ perspectives on quality aspects of burn care, which was used to translate their perspectives into patient-centred quality of care indicators. Qualitative descriptive research was conducted in a patient panel group. First, thematic analysis was applied to the focus groups to identify overarching themes. Second, patient-centred quality indicators, informed by burn survivors’ valued aspects of care, were defined. Ten burn survivors with an average age of 54 years (SD = 11; range 38–72 years) and mean TBSA burned of 14% (SD = 11%; range 5–35%) participated in two focus groups. Four overarching themes were identified, pointing to the importance of (1) information tailored to the different phases of recovery, (2) significant others’ wellbeing and involvement, (3) a therapeutic relationship and low-threshold access to healthcare professionals and (4) to participate in decision-making. Eighteen patient-centred process quality of care indicators within nine aspects of care were formulated. The overarching themes are reflected in patient-centred quality indicators, which present a broadened and complementary view of existing clinical quality indicators for burn care. Evaluating these patient-centred quality indicators may increase quality of care and refine patient-centred care.
Full article
Open AccessOpinion
Hypnosis in Burn Care: Efficacy, Applications, and Implications for Austere Settings
by
Deanna C. Denman
Eur. Burn J. 2024, 5(3), 207-214; https://doi.org/10.3390/ebj5030020 (registering DOI) - 1 Jul 2024
Abstract
Burn injuries are among the most traumatic events a person can endure, often causing significant psychological dysfunction and severe pain. Hypnosis shows promise as a complementary intervention to manage pain and reduce the psychological distress associated with burn injury and treatment. This paper
[...] Read more.
Burn injuries are among the most traumatic events a person can endure, often causing significant psychological dysfunction and severe pain. Hypnosis shows promise as a complementary intervention to manage pain and reduce the psychological distress associated with burn injury and treatment. This paper reviews the literature regarding hypnosis and potential applications of hypnosis in the management of burns. Hypnosis offers an effective, low-cost intervention that is widely applicable in the management of burns and can play a role in more acute and austere settings where resources are often limited.
Full article
(This article belongs to the Special Issue Burn Injuries Associated with Wars and Disasters)
Open AccessCase Report
Optimising Scar Management Intervention in the Case of a Head-and-Neck Burn for a Patient with a Learning Disability
by
Katie Spooner, Matthew Pilley, Liz Rose, Stephen Frost and Reena Agarwal
Eur. Burn J. 2024, 5(3), 198-206; https://doi.org/10.3390/ebj5030019 - 25 Jun 2024
Abstract
Scars following burns can often prove complex to manage, particularly when crossing joints or special areas such as the head and neck, due to contractures. This case report discusses the individualised care and rehabilitation provided to a burn patient with a learning disability.
[...] Read more.
Scars following burns can often prove complex to manage, particularly when crossing joints or special areas such as the head and neck, due to contractures. This case report discusses the individualised care and rehabilitation provided to a burn patient with a learning disability. The patient suffered both full and partial thickness burns equating to a total body surface area (%TBSA) of 7% of the face, neck, and anterior chest via the self-ignition of clothing. Acute treatment was provided at a regional burn unit followed by further in-patient care and rehabilitation at our burn facility. A motion rehabilitation instrument was employed to manage potential orofacial contracture; however, due to the patient’s impaired social functioning, this device was found to be unsuitable. Subsequently, a bespoke mouth-opening device replicating an ice lolly was fabricated utilising computer-aided design (CAD), enhancing the patient’s understanding along with encouraging independence. Microstomia was a risk in this case; however, this was prevented via the discussed regime, and successful patient rehabilitation was achieved.
Full article
Open AccessArticle
Person-Centred Pain Measurement in the ICU: A Multicentre Clinimetric Comparison Study of Pain Behaviour Observation Scales in Critically Ill Adult Patients with Burns
by
Alette E. E. de Jong, Wim E. Tuinebreijer, Helma W. C. Hofland and Nancy E. E. Van Loey
Eur. Burn J. 2024, 5(2), 187-197; https://doi.org/10.3390/ebj5020018 - 17 Jun 2024
Abstract
Pain in critically ill adults with burns should be assessed using structured pain behavioural observation measures. This study tested the clinimetric qualities and usability of the behaviour pain scale (BPS) and the critical-care pain observation tool (CPOT) in this population. This prospective observational
[...] Read more.
Pain in critically ill adults with burns should be assessed using structured pain behavioural observation measures. This study tested the clinimetric qualities and usability of the behaviour pain scale (BPS) and the critical-care pain observation tool (CPOT) in this population. This prospective observational cohort study included 132 nurses who rated pain behaviour in 75 patients. The majority of nurses indicated that BPS and CPOT reflect background and procedural pain-specific features (63–72 and 87–80%, respectively). All BPS and CPOT items loaded on one latent variable (≥0.70), except for compliance ventilator and vocalisation for CPOT (0.69 and 0.64, respectively). Internal consistency also met the criterion of ≥0.70 in ventilated and non-ventilated patients for both scales, except for non-ventilated patients observed by BPS (0.67). Intraclass correlation coefficients (ICCs) of total scores were sufficient (≥0.70), but decreased when patients had facial burns. In general, the scales were fast to administer and easy to understand. Cut-off scores for BPS and CPOT were 4 and 1, respectively. In conclusion, both scales seem valid, reliable, and useful for the measurement of acute pain in ICU patients with burns, including patients with facial burns. Cut-off scores associated with BPS and CPOT for the burn population allow professionals to connect total scores to person-centred treatment protocols.
Full article
Open AccessEditorial
European Burns Association (EBA)—Summer 2024 News
by
Stian Almeland, Nadia Depetris and on behalf of the European Burns Association Executive Board
Eur. Burn J. 2024, 5(2), 185-186; https://doi.org/10.3390/ebj5020017 - 14 Jun 2024
Abstract
The European Burns Association (EBA), as the proud owner of the European Burn Journal (EBJ), is committed to fostering collaboration and maximizing the impact of our common goals, i [...]
Full article
Open AccessArticle
Total Body Surface Area Adjusted Daily Diagnostic Blood Loss May Be Higher in Minor Burns—Are Our Patients the Victims of Daily Routine?
by
Christian Smolle, Anna Alexandra Elisabeth Persson, Caroline Lind and Fredrik Huss
Eur. Burn J. 2024, 5(2), 175-184; https://doi.org/10.3390/ebj5020016 - 6 Jun 2024
Abstract
►▼
Show Figures
Burns are common and devastating injuries, often necessitating intensive care treatment and long-term hospitalisation, making burn patients susceptible to hospital-acquired anaemia and blood transfusion. The purpose of this study was to assess diagnostic blood loss in burn patients at the burn intensive care
[...] Read more.
Burns are common and devastating injuries, often necessitating intensive care treatment and long-term hospitalisation, making burn patients susceptible to hospital-acquired anaemia and blood transfusion. The purpose of this study was to assess diagnostic blood loss in burn patients at the burn intensive care unit (BICU) at Uppsala University Hospital between 1 September 2016 and 30 June 2019. Medical records were screened; age, gender, mechanism, % total body surface area (TBSA), Baux score, length of stay, days on the respirator, days of continuous renal replacement therapy, number of operations, and number of blood tests per patient were assessed. Volume per blood test was estimated as the volume needed for the specific test tube. A total of 166 patients were included in the study. The mean TBSA was 18.0% ± 20, and the mean length of stay was 17.0 ± 41 days. Median diagnostic blood loss was 13.1 mL/day/patient (IQR 7.0, 23.9) and correlated positively with burn extent, Baux score, and mortality. Daily diagnostic blood loss/%TBSA/patient was 1.2 mL (IQR 0.7, 2.3). Transfusion of blood products occurred in 73/166 patients (44%). In conclusion, diagnostic blood loss is greatly influenced by TBSA extent. The diagnostic blood loss can reach significant levels and may affect the transfusion rate.
Full article

Figure 1
Open AccessCase Report
Management of Concomitant Severe Thermal Injury and ST-Elevation Myocardial Infarction
by
Julie Beveridge, Curtis Budden, Abelardo Medina, Kathryne Faccenda, Shawn X. Dodd and Edward Tredget
Eur. Burn J. 2024, 5(2), 169-174; https://doi.org/10.3390/ebj5020015 - 4 Jun 2024
Abstract
Acute coronary thrombosis is a known, but rare, contributor to morbidity and mortality in patients with thermal and electrical injuries. The overall incidence of myocardial infarction among burn patients is 1%, with an in-hospital post-infarction mortality of approximately 67%, whereas the overall mortality
[...] Read more.
Acute coronary thrombosis is a known, but rare, contributor to morbidity and mortality in patients with thermal and electrical injuries. The overall incidence of myocardial infarction among burn patients is 1%, with an in-hospital post-infarction mortality of approximately 67%, whereas the overall mortality rate of the general burn patient population is from 1.4% to 18%. As such, early detection and effective peri-operative management are essential to optimize patient outcomes. Here, we report the details of the management of an adult male patient with a 65% total body surface area severe thermal injury, who developed an ST-elevation myocardial infarction (STEMI) in the resuscitation period. The patient was found to have 100% occlusion of his left anterior descending coronary artery, for which prompt coronary artery stent placement with a drug-eluting stent (DES) was performed. Following stent placement, the patient required dual antiplatelet therapy. The ongoing dual antiplatelet therapy required the development of a detailed peri-operative protocol involving pooled platelets, packed red blood cells, desmopressin (DDAVP™) and intraoperative monitoring of the patient’s coagulation parameters with thromboelastography for three staged operative interventions to achieve complete debridement and skin grafting of his burn wounds.
Full article
Open AccessEditorial
Person and Family Centredness—The Need for Clarity of Focus
by
Brendan McCormack
Eur. Burn J. 2024, 5(2), 166-168; https://doi.org/10.3390/ebj5020014 - 27 May 2024
Abstract
Congratulations to the editorial team of the European Burn Journal for having the vision to host a Special Issue on the theme of “Person-Centred and Family-Centred Care Following Burn Injuries” [...]
Full article
(This article belongs to the Special Issue Person-Centered and Family-Centered Care Following Burn Injuries)
Open AccessArticle
An Optical Tomography-Based Score to Assess Pediatric Hand Burns
by
Judith Lindert, Tina Straube, Beke Larsen, Julia Siebert, Eirini Liodaki, Kianusch Tafazzoli-Lari and Lutz Wünsch
Eur. Burn J. 2024, 5(2), 155-165; https://doi.org/10.3390/ebj5020013 - 15 May 2024
Abstract
►▼
Show Figures
To define the morphologic pattern of pediatric hand burns as visualized via optical coherence tomography (OCT) and dynamic OCT (D-OCT). We designed a scoring system to assess the depths of burn wounds on pediatric hands and tested this score in our cohort of
[...] Read more.
To define the morphologic pattern of pediatric hand burns as visualized via optical coherence tomography (OCT) and dynamic OCT (D-OCT). We designed a scoring system to assess the depths of burn wounds on pediatric hands and tested this score in our cohort of children with burn injuries to the hand. Overall, 67 hand burns in 48 children (0–15 years) were prospectively examined. Scans were interpreted by two independent observers. Relevant OCT findings were surface irregularity, loss of epidermis, loss of dermal pattern (skin lines or papillary spots, loss of surface regularity and irregular vascular pattern of the plexus papillaris. Score values were calculated retrospectively. A score of 4 was associated with spontaneous healing without the need for skin grafting, with a positive predictive value of 97%. Deeper wounds with delayed healing and/or the need of skin grafting received a score of 5 or above, with an agreement of medical healing in 80% and a positive predictive value of 56%. OCT and D-OCT provide clinically useful additional information in cases of pediatric hand burns. The OCT burn score has the potential to support clinical decision making and, subsequently, improve clinical outcomes and shorten hospital stays.
Full article

Figure 1
Open AccessArticle
The Early Childhood Development of Pediatric Burn Patients
by
Maxime D. Cuijpers, Moniek Akkerman, Martin G. A. Baartmans, Paul P. M. van Zuijlen and Anouk Pijpe
Eur. Burn J. 2024, 5(2), 145-154; https://doi.org/10.3390/ebj5020012 - 14 May 2024
Abstract
►▼
Show Figures
Our study aimed to provide a description of the early childhood development of pediatric burn patients relative to Dutch reference values, using both pre- and post-burn data from the Dutch Development Instrument and the D-score. Data from the Dutch Development Instrument were
[...] Read more.
Our study aimed to provide a description of the early childhood development of pediatric burn patients relative to Dutch reference values, using both pre- and post-burn data from the Dutch Development Instrument and the D-score. Data from the Dutch Development Instrument were used to calculate the D-score and age-standardized D-score. Similar to a growth chart, the D-score was used to plot pediatric burn patients’ development relative to Dutch reference values for their age. Pediatric burn patients’ (n = 38) median age at the time of injury was 1.0 (1.0–2.0) years old. Burn size ranged from 1.0% to 36.0% of the total body surface area. Ninety-five percent (± 6.0%) of pediatric burn patients passed each of the age-appropriate developmental milestones at the target age. The mean age-standardized D-score was just above the Dutch average (+0.49 SD [0.18, 0.80]) and did not vary depending on sex (p = 0.06) or burn size (p = 0.41). In conclusion, among pediatric patients aged up to two-and-a-half years old, with non-full thickness burns, development was on track relative to the Dutch reference values. Our findings offer valuable first insights into the early childhood development of pediatric burn patients and may alleviate some parental concerns.
Full article

Figure 1
Open AccessArticle
Acute Surgical and Rehabilitation Management of Complex Hand Burns in Combat Casualties
by
Jill M. Cancio, Jonathan B. Lundy and Leopoldo C. Cancio
Eur. Burn J. 2024, 5(2), 126-144; https://doi.org/10.3390/ebj5020011 - 5 May 2024
Abstract
►▼
Show Figures
Burns are inevitable in modern warfare and have comprised between 5% and 20% of battlefield injuries. Involvement of the hands is the leading cause of postburn functional impairment. The purpose of this paper is to provide guidance on aspects of care necessary for
[...] Read more.
Burns are inevitable in modern warfare and have comprised between 5% and 20% of battlefield injuries. Involvement of the hands is the leading cause of postburn functional impairment. The purpose of this paper is to provide guidance on aspects of care necessary for the management of complex hand burns in a battlefield setting. Proper assessment and establishment of a comprehensive plan of care at the onset of injury help to ensure optimal functional outcomes in hand function. Basic treatment principles for the acutely burned hand include edema management; early wound coverage, including excision of the burn and skin grafting; early and aggressive hand therapy; and burn-scar contracture mitigation strategies.
Full article
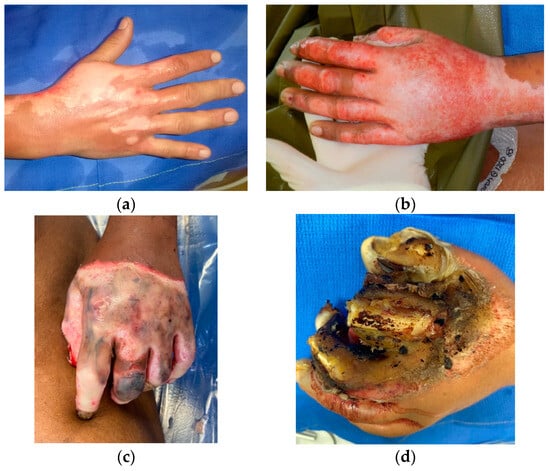
Figure 1
Open AccessArticle
Factors Associated with Self-Reported Voice Change in the Hospitalized Burn Population: A Burn Model System National Database Study
by
Kaitlyn L. Chacon, Edward Santos, Kara McMullen, Lauren J. Shepler, Carla Tierney-Hendricks, Audra T. Clark, Chiaka Akarichi, Haig A. Yenikomshian, Caitlin M. Orton, Colleen M. Ryan and Jeffrey C. Schneider
Eur. Burn J. 2024, 5(2), 116-125; https://doi.org/10.3390/ebj5020010 - 30 Apr 2024
Abstract
►▼
Show Figures
Voice plays a prominent role in verbal communication and social interactions. Acute burn care often includes intubation, mechanical ventilation, and tracheostomy, which could potentially impact voice quality. However, the issue of long-term dysphonia remains underexplored. This study investigates long-term self-reported voice changes in
[...] Read more.
Voice plays a prominent role in verbal communication and social interactions. Acute burn care often includes intubation, mechanical ventilation, and tracheostomy, which could potentially impact voice quality. However, the issue of long-term dysphonia remains underexplored. This study investigates long-term self-reported voice changes in individuals with burn injuries, focusing on the impact of acute burn care interventions. Analyzing data from a multicenter longitudinal database (2015–2023), self-reported vocal changes were examined at discharge and 6, 12, 24, and 60 months after injury. Out of 582 participants, 65 reported voice changes at 12 months. Changes were prevalent at discharge (16.4%) and persisted over 60 months (11.6–12.7%). Factors associated with voice changes included flame burn, inhalation injury, tracheostomy, outpatient speech-language pathology, head/neck burn, larger burn size, mechanical ventilation, and more ventilator days (p < 0.001). For those on a ventilator more than 21 days, 48.7% experience voice changes at 12 months and 83.3% had received a tracheostomy. The regression analysis demonstrates that individuals that were placed on a ventilator and received a tracheostomy were more likely to report a voice change at 12 months. This study emphasizes the need to understand the long-term voice effects of intubation and tracheostomy in burn care.
Full article
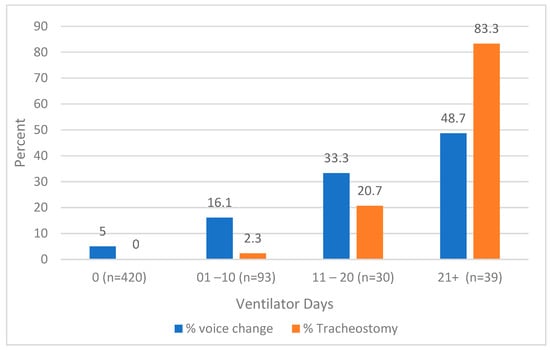
Figure 1
Open AccessArticle
Nonsteroidal Anti-Inflammatory Drugs Decrease Coagulopathy Incidence in Severe Burn Patients
by
Lyndon Huang, Kassandra Corona, Kendall Wermine, Elvia Villarreal, Giovanna De La Tejera, Phillip Howard Keys, Alen Palackic, Amina El Ayadi, George Golovko, Steven E. Wolf and Juquan Song
Eur. Burn J. 2024, 5(2), 104-115; https://doi.org/10.3390/ebj5020009 - 28 Apr 2024
Abstract
►▼
Show Figures
The study investigated the impact of nonsteroidal anti-inflammatory drugs (NSAIDs) on burn-induced coagulopathy in severely burned patients. Patients with a greater than 20% TBSA were identified in the TriNetX research network and categorized into receiving or not receiving NSAIDs in the first week
[...] Read more.
The study investigated the impact of nonsteroidal anti-inflammatory drugs (NSAIDs) on burn-induced coagulopathy in severely burned patients. Patients with a greater than 20% TBSA were identified in the TriNetX research network and categorized into receiving or not receiving NSAIDs in the first week after the burn. The statistical significance of the rate of burn-induced coagulopathy, mortality and sepsis in the week following injury was analysed. We observed 837 severely burned patients taking NSAIDS during the week following the burn and 1036 patients without. After matching for age, gender and race, the risk of burn-induced coagulopathy significantly decreased (p < 0.0001) in patients taking NSAIDs (17.7%) compared to those without (32.3%). Patients taking NSAIDs were also less likely to develop sepsis (p < 0.01) and thrombocytopenia (p < 0.001) or die the week following injury (p < 0.0001). In conclusion, the early protective effects of NSAIDs at reducing the risk of coagulopathy as well as sepsis and mortality occur during the acute phase of burns.
Full article
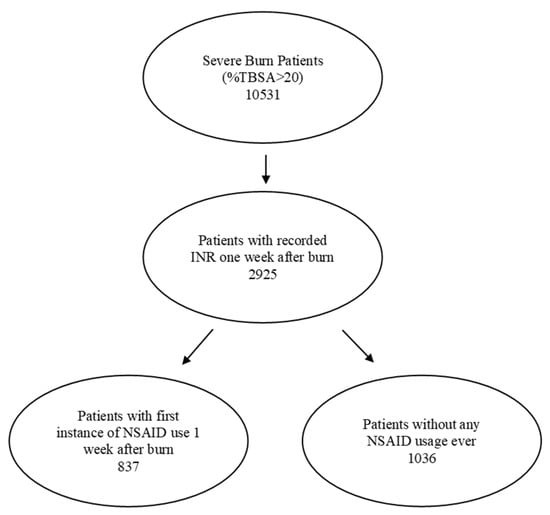
Figure 1
Open AccessArticle
Development and Testing of the Aftercare Problem List, a Burn Aftercare Screening Instrument
by
Nancy E. E. Van Loey, Elise Boersma-van Dam, Anita Boekelaar, Anneke van de Steenoven, Alette E. E. de Jong and Helma W. C. Hofland
Eur. Burn J. 2024, 5(2), 90-103; https://doi.org/10.3390/ebj5020008 - 29 Mar 2024
Abstract
A growing interest in person-centered care from a biopsychosocial perspective has led to increased attention to structural screening. The aim of this study was to develop an easy-to-comprehend screening instrument using single items to identify a broad range of health-related problems in adult
[...] Read more.
A growing interest in person-centered care from a biopsychosocial perspective has led to increased attention to structural screening. The aim of this study was to develop an easy-to-comprehend screening instrument using single items to identify a broad range of health-related problems in adult burn survivors. This study builds on earlier work regarding content generation. Focus groups and expert meetings with healthcare providers informed content refinement, resulting in the Aftercare Problem List (APL). The instrument consists of 43 items divided into nine health domains: scars, daily life functioning, scars treatment, body perceptions, stigmatization, intimacy, mental health, relationships, financial concerns, and a positive co** domain. The APL also includes a Distress Thermometer and a question inquiring about preference to discuss the results with a healthcare provider. Subsequently, the APL was completed by 102 outpatients. To test face validity, a linear regression analysis showed that problems in three health domains, i.e., scars, mental health, and body perceptions, were significantly related to higher distress. Qualitative results revealed that a minority found the items difficult which led to further adjustment of the wording and the addition of illustrations. In summation, this study subscribes to the validity of using single items to screen for burn-related problems.
Full article
(This article belongs to the Special Issue Person-Centered and Family-Centered Care Following Burn Injuries)
►▼
Show Figures

Figure 1
Open AccessArticle
Parental Stress and Child Quality of Life after Pediatric Burn
by
Dinithi Atapattu, Victoria M. Shoesmith, Fiona M. Wood and Lisa J. Martin
Eur. Burn J. 2024, 5(2), 77-89; https://doi.org/10.3390/ebj5020007 - 27 Mar 2024
Abstract
Parents’ emotions after their child’s burn might be influenced by the injury circumstances or demographic characteristics of the patient and family. Parents’ post-traumatic stress symptoms and their child’s distress may interact and affect emotional states. The psychosocial outcomes of parents were measured using
[...] Read more.
Parents’ emotions after their child’s burn might be influenced by the injury circumstances or demographic characteristics of the patient and family. Parents’ post-traumatic stress symptoms and their child’s distress may interact and affect emotional states. The psychosocial outcomes of parents were measured using the Impact of Event Scale-Revised, the CARe Burn Scale, and the Post-traumatic Growth Inventory-Brief. The psychosocial quality of life outcomes of the pediatric burn patients were measured using the Pediatric Quality of Life Inventory (PedsQL). Regression analysis was used to assess the relationship between patient psychosocial quality of life and the related parent scores. A total of 48 patients and parents participated, with 36 giving full data at 12 months. Parental post-traumatic stress symptoms were initially high, settling by six months, although outliers remained. Parents reported higher IESR scores if their child was female, if they felt helpless at the time of the incident, and if a language other than English was spoken in the home. Parents’ scores of their child’s psychosocial function were similar to their child’s self-scores. Parents who perceived poorer emotional functioning in their child reported higher IESR scores.
Full article
(This article belongs to the Special Issue Person-Centered and Family-Centered Care Following Burn Injuries)
►▼
Show Figures

Figure 1
Open AccessReview
Extracorporeal Organ Support for Burn-Injured Patients
by
Garrett W. Britton, Amanda R. Keith, Barret J. Halgas, Joshua M. Boster, Nicholas S. Niazi, Kevin K. Chung and Leopoldo C. Cancio
Eur. Burn J. 2024, 5(2), 66-76; https://doi.org/10.3390/ebj5020006 - 25 Mar 2024
Abstract
As mortality relating to severe acute burn injury improves, patients are surviving longer into the critical care phase, which is commonly complicated by multisystem organ failure. Extracorporeal organ support (ECOS) represents a set of potential therapeutic technologies for managing patients with organ-specific complications.
[...] Read more.
As mortality relating to severe acute burn injury improves, patients are surviving longer into the critical care phase, which is commonly complicated by multisystem organ failure. Extracorporeal organ support (ECOS) represents a set of potential therapeutic technologies for managing patients with organ-specific complications. This article provides a comprehensive review of the existing literature, focusing on the use of continuous kidney replacement therapy, extracorporeal membrane oxygenation, extracorporeal carbon dioxide removal, and extracorporeal blood purification. Though promising, many of these technologies are in the early phases of implementation and are restricted to well-resourced medical systems, limiting their use in large scale casualty and austere scenarios.
Full article
(This article belongs to the Special Issue Burn Injuries Associated with Wars and Disasters)
Open AccessReview
Burn Wound Care Strategies for the Battlefield and Austere Settings
by
Sarah Shingleton, Jared Folwell, Ian Jones, Michael Gleason and Alicia Williams
Eur. Burn J. 2024, 5(1), 49-65; https://doi.org/10.3390/ebj5010005 - 23 Feb 2024
Abstract
Burns are commonly encountered in the battlefield environment; however, the availability of burn expertise and specialized supplies is variable. Initial burn care should remain focused on cooling the burn, preventing hypothermia, basic wound cleansing, and evacuation. Key ongoing burn wound management principles include
[...] Read more.
Burns are commonly encountered in the battlefield environment; however, the availability of burn expertise and specialized supplies is variable. Initial burn care should remain focused on cooling the burn, preventing hypothermia, basic wound cleansing, and evacuation. Key ongoing burn wound management principles include wound debridement, accurate burn size and depth estimation, wound care, ongoing wound evaluation, and treatment of suspected Gram-negative wound infection. Operative management should be limited to urgent procedures, and definitive burn management should be performed only after evacuation to a higher level of care. Flexibility, creativity, and the ability to adapt care to the tactical environment are key to the successful management of burn injuries in battlefield and austere settings.
Full article
(This article belongs to the Special Issue Burn Injuries Associated with Wars and Disasters)
Open AccessFeature PaperArticle
Comparison of Clinical Estimation and Stereophotogrammic Instrumented Imaging of Burn Scar Height and Volume
by
Shyla Kajal Bharadia and Vincent Gabriel
Eur. Burn J. 2024, 5(1), 38-48; https://doi.org/10.3390/ebj5010004 - 12 Feb 2024
Abstract
►▼
Show Figures
Descriptive clinical tools for characterizing burn scars are limited by between-user variability and unknown sensitivity to change over time. We previously described preclinical assessment of stereophotogrammetry as a valid measure of burn-related scars. Here, we compared the estimated vs. instrumented measurements of maximum
[...] Read more.
Descriptive clinical tools for characterizing burn scars are limited by between-user variability and unknown sensitivity to change over time. We previously described preclinical assessment of stereophotogrammetry as a valid measure of burn-related scars. Here, we compared the estimated vs. instrumented measurements of maximum height and total positive volume of 26 burn scars. The burn scars were imaged with the QuantifiCare LifeViz Micro 3D camera. Three experienced wound care therapists first estimated, then measured using 3D Track software, the imaged scars’ height and volume. Two-factor analysis without replication was performed to calculate intraclass correlation coefficients (ICCs) between assessors’ estimated scar height and volume, and measured height and volume. Two-sided Wilcoxon tests were performed comparing the mean estimated height and volume with the estimated and measured outputs. The estimated scar height’s ICC was 0.595, and for volume, it was 0.531. The measured scar height’s ICC was 0.933 and for volume, it was 0.890. The estimated and measured volume were significantly different (z = −2.87, p = 0.041), while the estimated and measured height were not (z = −1.39, p = 0.161). Stereophotogrammic measurement of scar height and volume is more reliable than clinical photograph assessment. Stereophotogrammetry should be utilized when assessing burn scar height and volume, rather than subjective estimates from clinical scar tools.
Full article

Figure 1
Open AccessReview
Enteral Resuscitation: A Field-Expedient Treatment Strategy for Burn Shock during Wartime and in Other Austere Settings
by
Ian F. Jones, Kiran Nakarmi, Hannah B. Wild, Kwesi Nsaful, Kajal Mehta, Raslina Shrestha, Daniel Roubik and Barclay T. Stewart
Eur. Burn J. 2024, 5(1), 23-37; https://doi.org/10.3390/ebj5010003 - 18 Jan 2024
Abstract
Burn injuries are a constant threat in war. Aspects of the modern battlefield increase the risk of burn injuries and pose challenges for early treatment. The initial resuscitation of a severely burn-injured patient often exceeds the resources available in front-line medical facilities. This
[...] Read more.
Burn injuries are a constant threat in war. Aspects of the modern battlefield increase the risk of burn injuries and pose challenges for early treatment. The initial resuscitation of a severely burn-injured patient often exceeds the resources available in front-line medical facilities. This stems mostly from the weight and volume of the intravenous fluids required. One promising solution to this problem is enteral resuscitation with an oral rehydration solution. In addition to being logistically easier to manage, enteral resuscitation may be able to mitigate secondary injuries to the gut related to burn shock and systemic immunoinflammatory activation. This has been previously studied in burn patients, primarily using electrolyte solutions, with promising results. Modern ORS containing sodium, potassium, and glucose in ratios that maximize gut absorption may provide additional benefits as a resuscitation strategy, both in terms of plasma volume expansion and protection of the barrier and immune functions of the gut mucosa. While enteral resuscitation is promising and should be used when other options are not available, further research is needed to refine an optimal implementation strategy.
Full article
(This article belongs to the Special Issue Burn Injuries Associated with Wars and Disasters)
►▼
Show Figures

Figure 1
Open AccessArticle
Combat and Operational Stress Control: Application in a Burn Center
by
Jill M. Cancio and Leopoldo C. Cancio
Eur. Burn J. 2024, 5(1), 12-22; https://doi.org/10.3390/ebj5010002 - 29 Dec 2023
Abstract
Occupational therapy has been integral to the holistic recovery of soldiers since its origin. The positive psychosocial and physiological effects of occupation-based interventions, fundamental to the profession, have long justified its relevance to the military. As such, occupational therapy has been written into
[...] Read more.
Occupational therapy has been integral to the holistic recovery of soldiers since its origin. The positive psychosocial and physiological effects of occupation-based interventions, fundamental to the profession, have long justified its relevance to the military. As such, occupational therapy has been written into US Army doctrine as an integral component of the Combat and Operational Stress Control (COSC) program. The focus of a COSC unit is to prevent, identify, reduce, and manage combat and operational stress reactions resulting from physical and mental stressors in a combat environment. COSC centers around the recognition and resolution of functional problems and the development of enhanced co** skills. Recognizing that burn patients are, like combatants, also at high risk of stress-related illness, we applied COSC concepts to peacetime burn care. In this paper we describe the theoretical basis for COSC in a burn center. The COSC model supports holistic, functional recovery of the burn casualty and can augment psychosocial recovery, particularly in times of limited resources.
Full article
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics

Conferences
Special Issues
Special Issue in
EBJ
Enhancing Burn Rehabilitation: Contemporary Improvements across the Spectrum of Influence
Guest Editors: Dale Edgar, Colleen Ryan, Marianne K. Nieuwenhuis, Ulrike Van Daele, Jill CancioDeadline: 1 September 2024
Special Issue in
EBJ
Long-Term Outcomes after Burn Injuries: Strategies to Optimize Recovery
Guest Editors: Nicole S. Gibran, Haig Yenikomshian, Gretchen Carrougher, Samuel MandellDeadline: 31 December 2024
Special Issue in
EBJ
Controversial Issues in Intensive Care-Related Burn Injuries
Guest Editor: Athina LavrentievaDeadline: 30 April 2025
Special Issue in
EBJ
Global Perspectives on Burn Prevention, Management, Collaboration, and Disparities
Guest Editor: Laura PompermaierDeadline: 31 May 2025