Journal Description
Pediatric Reports
Pediatric Reports
is an international, scientific, peer-reviewed open access journal on all aspects of pediatrics, published quarterly online by MDPI (from Volume 12 Issue 3 - 2020). The Italian Society of Pediatric Psychology (SIPPed) is affiliated with Pediatric Reports and the members receive discounts of the article processing charge.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, ESCI (Web of Science), PubMed, PMC, Embase, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 29.6 days after submission; acceptance to publication is undertaken in 4.6 days (median values for papers published in this journal in the first half of 2024).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Impact Factor:
1.4 (2023);
5-Year Impact Factor:
1.2 (2023)
Latest Articles
Acquired Zinc Deficiency in Preterm Infant Post-Surgery for Necrotizing Enterocolitis (NEC) on Prolonged Total Parenteral Nutrition (TPN)
Pediatr. Rep. 2024, 16(3), 551-557; https://doi.org/10.3390/pediatric16030046 - 26 Jun 2024
Abstract
Zinc (Zn) is a vital trace element that plays a pivotal role in protein synthesis, cellular growth, and differentiation and is involved as a cofactor of metalloenzymes, performing a wide variety of metabolic, immune, and synthesis roles. Zn is required at all stages
[...] Read more.
Zinc (Zn) is a vital trace element that plays a pivotal role in protein synthesis, cellular growth, and differentiation and is involved as a cofactor of metalloenzymes, performing a wide variety of metabolic, immune, and synthesis roles. Zn is required at all stages of an infant’s and child’s development, and severe Zn deficiency has been reported to lead to slower physical, cognitive, and sexual growth. Preterm neonates are at a higher risk of develo** zinc deficiency for a variety of reasons, including low Zn intake from enteral feeds containing breast milk, relative malabsorption due to immaturity of the gastrointestinal tract with limited absorptive capacity, increased urinary loss of zinc, and increased demand during the early developmental stages. Moreover, premature infants are at risk of gastrointestinal diseases like necrotizing enterocolitis (NEC), which can limit absorption capacity and potentially lead to malabsorption. TPN is frequently used in preterm infants to provide them with sufficient nutrients and calories. However, it has its own complications, including cholestasis, especially if used for prolonged periods. In this case report, we are presenting the case of a male preterm infant who was delivered by caesarean section at 26 weeks’ gestation. The baby developed an intestinal perforation due to NEC, for which he underwent surgery for resection of the necrotic bowel and the creation of a high ileal stoma and was put on prolonged total parenteral nutrition (TPN), which led to the development of zinc deficiency.
Full article
Open AccessArticle
Is It Safe to Operate without Frozen Section Biopsies in Short-Segment Hirschsprung’s Disease? An Overview of 60 Cases
by
Isber Ademaj, Nexhmi Hyseni and Naser Gjonbalaj
Pediatr. Rep. 2024, 16(3), 542-550; https://doi.org/10.3390/pediatric16030045 - 25 Jun 2024
Abstract
Background: Advancements in surgical management in a single-stage procedure made intraoperative frozen section biopsies critical for determining of level of resection to avoid the potential risk of leaving a retained aganglionic segment. However, in most low-income countries, due to the lack of this
[...] Read more.
Background: Advancements in surgical management in a single-stage procedure made intraoperative frozen section biopsies critical for determining of level of resection to avoid the potential risk of leaving a retained aganglionic segment. However, in most low-income countries, due to the lack of this facility, the surgeon’s intraoperative judgment is used for the determination of the resection level. Objective: This study aims to evaluate the accuracy of determining the level of bowel resection in short-segment Hirschsprung’s disease based on macroscopic changes. Materials and methods: Intraoperative macroscopic evaluations were assessed using postoperative microscopic findings to determine whether the surgeons’ intraoperative judgments were accurate in determining the level of bowel resection in 60 cases of operated short-segment Hirschsprung’s disease. In addition, Pearson’s correlation coefficient was used to determine whether the sensitivity and specificity of both methods were significantly correlated. Results: The microscopic results showed that the level of resection based on the macroscopic evaluation was performed in normally ganglionated segment in cases of short-segment Hirschsprung’s disease. Conclusion: Macroscopic intraoperative assessment by an experienced surgeon is highly accurate method of determining the level of bowel resection in short-segment HSCR.
Full article
Open AccessArticle
Respiratory Symptoms among Adolescents in Poland: A Study on Cigarette Smokers, E-Cigarette Users, and Dual Users
by
Paulina Kurdyś-Bykowska, Leon Kośmider, Dawid Konwant and Krystyna Stencel-Gabriel
Pediatr. Rep. 2024, 16(3), 530-541; https://doi.org/10.3390/pediatric16030044 - 21 Jun 2024
Abstract
In recent years, the prevalence of tobacco and electronic cigarette (e-cigarette) use among adolescents has raised significant public health concerns worldwide. This study aimed to investigate respiratory symptoms among Polish adolescents. We conducted an online survey among Polish school students from all provinces,
[...] Read more.
In recent years, the prevalence of tobacco and electronic cigarette (e-cigarette) use among adolescents has raised significant public health concerns worldwide. This study aimed to investigate respiratory symptoms among Polish adolescents. We conducted an online survey among Polish school students from all provinces, collecting data over two months in spring 2021. Students voluntarily complete the anonymous survey, answering questions about respiratory symptoms, smoking habits (both traditional and electronic cigarettes), and demographic information. The analysis focused on four subgroups, namely non-tobacco users, traditional cigarette smokers, e-cigarette users, and dual users, totaling 10,388 pupils aged 12–18 years, predominantly attending secondary technical and comprehensive schools. A total of 10,388 pupils participated in the study, 55.6% (5778) of whom were girls and 44.4% (4610) boys. Adolescents who admitted using both e-cigarettes and traditional cigarettes experienced more frequent episodes of cough during the day (39.70%) and at night (18.40%) compared to their peers in other groups. Chest discomfort, including pain and pressure, was also reported more often by adolescents who used e-cigarettes and traditional cigarettes concurrently (27.60%) compared to their peers in other groups. Chest pressure was experienced less commonly by non-smoking adolescents (14.40%) than by smokers (18.90%). Higher severity of cough during the day and at night was observed in the group of adolescents using traditional cigarettes and e-cigarettes concurrently compared to the other groups. The adolescents in the dual-user group experienced more severe dyspnea and wheezing compared to the other groups included in the comparison. The results of this study confirm the correlation between the occurrence of respiratory symptoms in adolescents who smoke cigarettes, adolescents who use e-cigarettes, and adolescents who are dual users. The respiratory symptoms occur most frequently and are the most severe in the group of adolescents who use e-cigarettes and traditional cigarettes.
Full article
Open AccessArticle
The Psychosocial Impact of the COVID-19 Pandemic on Italian Families: The Perception of Quality of Life and Screening of Psychological Symptoms
by
Roberta Maria Incardona and Marta Tremolada
Pediatr. Rep. 2024, 16(2), 519-529; https://doi.org/10.3390/pediatric16020043 - 20 Jun 2024
Abstract
Throughout the COVID-19 period, families were forced to stay indoors, adapting to online schooling, remote work, and virtual social engagements, inevitably altering the dynamics within households. There was a notable increase in mental health challenges in terms of anxiety and depression in children
[...] Read more.
Throughout the COVID-19 period, families were forced to stay indoors, adapting to online schooling, remote work, and virtual social engagements, inevitably altering the dynamics within households. There was a notable increase in mental health challenges in terms of anxiety and depression in children and adolescents. This study intended to explore the psychosocial effects of the COVID-19 pandemic on Italian families by adopting self- and proxy-report questionnaires on anxiety, anger, and health-related quality of life. The results showed that approximately 20% obtained a clinical anxiety score and only 10% obtained a clinical anger score. There was a difference in the perception of the quality of life reported by the child and that perceived by the parent. A stepwise regression model showed that total anxiety scores were predicted by sex, quality of life scores from the parents’ self-report version, and the total anger score. Another stepwise regression model identified physiological and social anxiety as the best predictors that impact quality of life. Parental well-being actively influences the well-being of children, so it is fundamental to implement preventive programs and promote child well-being by providing parents the most adequate support possible.
Full article
(This article belongs to the Special Issue Mental Health and Psychiatric Disorders of Children and Adolescents)
►▼
Show Figures

Figure 1
Open AccessReview
Foreign Bodies in Pediatric Otorhinolaryngology: A Review
by
Ivan Paladin, Ivan Mizdrak, Mirko Gabelica, Nikolina Golec Parčina, Ivan Mimica and Franko Batinović
Pediatr. Rep. 2024, 16(2), 504-518; https://doi.org/10.3390/pediatric16020042 - 19 Jun 2024
Abstract
►▼
Show Figures
Foreign bodies (FBs) in pediatric otorhinolaryngology represent up to 10% of cases in emergency departments (ED) and are primarily present in children under five years old. They are probably the result of children’s curiosity and tendency to explore the environment. Aural and nasal
[...] Read more.
Foreign bodies (FBs) in pediatric otorhinolaryngology represent up to 10% of cases in emergency departments (ED) and are primarily present in children under five years old. They are probably the result of children’s curiosity and tendency to explore the environment. Aural and nasal FBs are the most common and accessible, and the removal methods differ depending on the exact location and type of FB, which can be organic or inorganic. A fish bone stuck in one of the palatine tonsils is the most common pharyngeal FB. Laryngopharyngeal FBs can obstruct the upper respiratory tract and thus become acutely life-threatening, requiring an urgent response. Aspiration of FBs is common in children between 1 and 4 years old. A history of coughing and choking is an indication of diagnostic and therapeutic methods to rule out or confirm a tracheobronchial FB. Regardless of the availability of radiological diagnostics, rigid bronchoscopy is the diagnostic and therapeutic method of choice in symptomatic cases. Radiological diagnostics are more significant in treating esophageal FBs since most are radiopaque. Flexible or rigid esophagoscopy is a successful method of removal. A delayed diagnosis, as with tracheobronchial FBs, can lead to fatal consequences.
Full article

Figure 1
Open AccessArticle
Clinical Study and Microbiological Analysis of Periodontopathogenic Microflora Analyzed among Children and Adolescents with Cardiovascular Diseases Compared to Group with Good General Status
by
Oana Chipirliu, Marian Viorel Crăciun and Madalina Nicoleta Matei
Pediatr. Rep. 2024, 16(2), 482-503; https://doi.org/10.3390/pediatric16020041 - 18 Jun 2024
Abstract
Periodontal diseases, as an important part of oral pathology, present different characteristics when affecting children and adolescents or young adults. Studies have shown that adolescence and childhood are closely related to a high risk of periodontal disease, but the follow-up for periodontal health
[...] Read more.
Periodontal diseases, as an important part of oral pathology, present different characteristics when affecting children and adolescents or young adults. Studies have shown that adolescence and childhood are closely related to a high risk of periodontal disease, but the follow-up for periodontal health or damage at this age has been insufficiently appreciated until now. The aim of this study was to identify subgingival microorganisms using a real-time polymerase chain reaction (PCR) in a group of children and adolescents aged 7–17 years with and without cardiovascular disease. The group of 62 subjects with gingival inflammation and poor hygiene was divided into two groups according to general condition: 31 subjects with carduivascular disease (group A) and 31 subjects without cardiovascular disease (group C). Subjects were examined in the initial consultation, the state of hygiene and periodontal inflammation was assessed using the plaque index (PI) and gingival index (GI), and samples were taken from the gingival sulcus using sterile paper cones to determine nine subgingival microorganisms. Nine subgingival microorganisms were identified: Aggregatibacter actinomycetemcomitans (Aa), Porphyromonas gingivalis (Pg), Treponema denticola (Td), Tannerella forsythias (Tf), Prevotella intermedia (Pi), Peptostreptococcus (Micromonas) micros (Pm), Fusobacterium nucleatum (Fn), Eubacterium nodatum (En), and Capnocytophaga gingivalis (Cg). The patients were included in a specialist treatment program which aimed to relieve the inflammatory condition, remove local irritative factors, and train the patients to perform proper oral hygiene at home by using primary and secondary oral hygiene products. Subjects were reevaluated 3 months after treatment, when measurements for the PI and GI and microbiological determinations were repeated. The results showed a predominance of subjects aged 16–17 years (12.4%). Among the subjects with marked gingival inflammation, the male gender was predominant (58.06%). The PI values changed considerably after treatment, with lower values in patients presenting a general condition without cardiovascular disease (PI = 8.10%) compared with the patients with cardiovascular disease (PI = 13.77%). After treatment, the GI showed considerable changes in both groups. Red, orange, and purple complex microorganisms were found before treatment and decreased considerably after treatment in both groups. The highest values were found for Treponema denticola (140,000 (1.4 × 105)) in patients with cardiovascular disease and generalized gingival inflammation. Of the pathogenic microorganisms, the most common was Tannerella forsythia in 52 patients before treatment, and red microorganisms considerably appeared in only 10 patients after treatment. Capnocytophaga gingivalis remained constant both in the diseased state and after treatment and was consistent with periodontal health. Children with cardiovascular diseases had a higher prevalence of gingival manifestations. The composition of the subgingival microbial plaque was directly influenced by the degree of oral hygiene, but the response to specialized treatment was also influenced by the general health status. The results of this study support the conclusion that periodontal pathogens appear and multiply in the absence of proper hygiene in childhood after the eruption of permanent teeth, and their action leads to the initiation of periodontal diseases.
Full article
(This article belongs to the Special Issue Modern Solutions for Diagnosis and Treatment Planning in Pediatric Dentistry and Orthodontics)
►▼
Show Figures

Figure 1
Open AccessSystematic Review
Impact of Adverse Childhood Experiences in Young Adults and Adults: A Systematic Literature Review
by
Candy Silva, Patrícia Moreira, Diana Sá Moreira, Filipa Rafael, Anabela Rodrigues, Ângela Leite, Sílvia Lopes and Diana Moreira
Pediatr. Rep. 2024, 16(2), 461-481; https://doi.org/10.3390/pediatric16020040 - 7 Jun 2024
Abstract
►▼
Show Figures
Background: Investigations have shown the different impacts that ACEs have on an individual’s adult life, on both physical and mental health, but they have not yet shown the issue of the influence of ACEs on adults and young adults. Objective/Participants and Setting: This
[...] Read more.
Background: Investigations have shown the different impacts that ACEs have on an individual’s adult life, on both physical and mental health, but they have not yet shown the issue of the influence of ACEs on adults and young adults. Objective/Participants and Setting: This systematic review, performed according to the PRISMA norms and guidelines, intended to understand the most frequent outcomes of adverse childhood experiences in the life of young adults and adults. Methods: Studies were identified through multiple literature search databases at EBSCOhost, Web of Science, and PubMed April 2023, and a total of 279 studies, published between 1999 and 2002, were excluded, 256 because of multiple factors: being duplicates, showing statistical analysis with correlations only, being systematic reviews or case studies, comprising individuals under the age of 18, and not meeting the intended theme; ultimately, we selected for the review a total of 23 studies. Results and Conclusions: The impacts of the various articles are subdivided into three main themes: antisocial and criminal behaviour; sexual Behaviour and intimate partner violence; and attachment, quality of life, and therapeutic alliance.
Full article

Figure 1
Open AccessArticle
Impact of COVID-19 Pandemic on the Clinical Course and Complications of Varicella—A Retrospective Cohort Study
by
Maja Pietrzak and Maria Pokorska-Śpiewak
Pediatr. Rep. 2024, 16(2), 451-460; https://doi.org/10.3390/pediatric16020039 - 4 Jun 2024
Abstract
In this study, we aimed to characterize a cohort of children hospitalized due to varicella before and after the outbreak of the COVID-19 pandemic. Medical charts of all children hospitalized in the Regional Hospital of Infectious Diseases in Warsaw due to varicella in
[...] Read more.
In this study, we aimed to characterize a cohort of children hospitalized due to varicella before and after the outbreak of the COVID-19 pandemic. Medical charts of all children hospitalized in the Regional Hospital of Infectious Diseases in Warsaw due to varicella in the years 2019 and 2022 were retrospectively analyzed and compared. In total, 221 children were included in the analysis; 59 of them were hospitalized in 2019, whereas 162 were hospitalized in 2022. Children hospitalized in 2022 were older than those reported in 2019 (median 4.0 vs. 3.0 years, p = 0.02). None of the hospitalized children received complete varicella vaccination. The most common complication in both years was bacterial superinfection of skin lesions, found in 156/221 (70.6%) of patients. This complication rate was higher in 2022 (50.8% in 2019 vs. 77.8% in 2022, p = 0.0001), OR = 3.38, 95% CI: 1.80–6.35. Moreover, skin infections in 2022 more often manifested with cellulitis (in 2022 13.6% vs. 3.4% in 2019, p = 0.03), OR = 4.40, 95% CI: 1.00–19.33. Sepsis as a complication of varicella was almost five-fold more prevalent in 2022 than in 2019 (p = 0.009), OR = 5.70, 95% CI: 1.31–24.77. Antibiotic use increased between 2019 and 2022 (71.2% vs. 85.2%, p = 0.01). Furthermore, patients were treated more frequently with the combination of two different antibiotics simultaneously (only 3.4% of patients in 2019 compared to 15.4% in 2022, p = 0.01). Primary infections with varicella zoster virus in 2022 led to a more severe course of the disease.
Full article
(This article belongs to the Collection COVID-19: What Happens in Pediatric Research in the Era of Pandemic)
►▼
Show Figures

Figure 1
Open AccessArticle
Analysis of Pediatric Pulpotomy, Pulpectomy, and Extractions in Primary Teeth Revealed No Significant Association with Subsequent Root Canal Therapy and Extractions in Permanent Teeth: A Retrospective Study
by
Arash Farhadian, Mayce Arreem Issa, Karl Kingsley and Victoria Sullivan
Pediatr. Rep. 2024, 16(2), 438-450; https://doi.org/10.3390/pediatric16020038 - 31 May 2024
Abstract
Recent evidence suggests that an ever-growing number of pediatric patients require invasive treatments such as root canal therapy (RCT) in their permanent dentition, albeit with little information about risk factors such as prior invasive treatments of pulpotomy or pulpectomy in their primary dentition.
[...] Read more.
Recent evidence suggests that an ever-growing number of pediatric patients require invasive treatments such as root canal therapy (RCT) in their permanent dentition, albeit with little information about risk factors such as prior invasive treatments of pulpotomy or pulpectomy in their primary dentition. Therefore, the primary objectives of this study were to determine the number of pediatric patients who have had any type of invasive treatment in their primary teeth, to assess their association with any subsequent invasive treatment (root canal therapy, extractions) in their permanent dentition, and to assess these trends over time. This retrospective study utilized summary data from a clinical pediatric patient pool (ages 0–17) over the period of 2013–2022. This analysis revealed that pediatric patients requiring pulpotomies and pulpectomies in primary dentition declined between 2013 (n = 417, n = 156) and 2022 (n = 250, n = 12), while root canal therapy (RCT) in permanent dentition increased six-fold from n = 54 to n = 330. In addition, few (7.8%) patients with RCT had a previous history of pulpotomy or pulpectomy, which suggests that invasive treatments performed in primary dentition have no direct association with the subsequent need for invasive treatments in permanent dentition, although more research is needed to determine the explanations for these observations.
Full article
(This article belongs to the Special Issue Modern Solutions for Diagnosis and Treatment Planning in Pediatric Dentistry and Orthodontics)
►▼
Show Figures

Figure 1
Open AccessCase Report
Chromosomal Integration of HHV-6 in a Preterm Neonate: A Rare Case of Hyperleukocytosis and Clinical Implications
by
Palanikumar Balasundaram and Mohamed Sakr
Pediatr. Rep. 2024, 16(2), 432-437; https://doi.org/10.3390/pediatric16020037 - 31 May 2024
Abstract
►▼
Show Figures
Leukocytosis in neonates can occur because of infectious, inflammatory, malignant, or physiological processes. Hyperleukocytosis is defined as a total leukocyte count (TLC) exceeding 100,000 per mm3, warranting immediate evaluation. Neonates with hyperleukocytosis are at risk of leukostasis and the associated severe
[...] Read more.
Leukocytosis in neonates can occur because of infectious, inflammatory, malignant, or physiological processes. Hyperleukocytosis is defined as a total leukocyte count (TLC) exceeding 100,000 per mm3, warranting immediate evaluation. Neonates with hyperleukocytosis are at risk of leukostasis and the associated severe complications, including respiratory distress, myocardial ischemia, hyperuricemia, acute renal failure, infarction, and hemorrhage. Differentiating leukemia and leukemoid reactions in neonates presenting with elevated TLC is challenging but critical. We present a unique case of a preterm male neonate with hyperleukocytosis, initially suspected to have an underlying malignancy. The neonate’s clinical course was complicated by respiratory distress syndrome and anemia of prematurity, necessitating neonatal intensive care unit management. Further investigation revealed high human herpesvirus 6 (HHV-6) DNA levels in the whole blood, leading to a chromosomally integrated HHV-6 (ciHHV-6) diagnosis. CiHHV-6 is characterized by HHV-6 DNA integration into the host genome. Accurate diagnosis relies on whole-blood quantitative PCR, distinguishing ciHHV-6 from an active infection. The neonate remained asymptomatic, and antiviral treatment was deemed unnecessary. This case underscores the importance of recognizing ciHHV-6 as a potential cause of hyperleukocytosis in neonates and highlights the value of whole-blood PCR for differentiation. Understanding the spectrum of HHV-6 infection in neonates is vital for appropriate management and prognostication.
Full article

Figure 1
Open AccessReview
Understanding the Neuropsychological Implications of Klinefelter Syndrome in Pediatric Populations: Current Perspectives
by
Panagiota Tragantzopoulou and Vaitsa Giannouli
Pediatr. Rep. 2024, 16(2), 420-431; https://doi.org/10.3390/pediatric16020036 - 25 May 2024
Abstract
Klinefelter syndrome (KS), also known as 47,XXY, is a genetic disorder characterized by the presence of an extra X chromosome. Despite the prevalence of verbal learning disabilities, memory impairments, and executive function deficits in individuals with KS, comprehensive research on the neuropsychological profiles
[...] Read more.
Klinefelter syndrome (KS), also known as 47,XXY, is a genetic disorder characterized by the presence of an extra X chromosome. Despite the prevalence of verbal learning disabilities, memory impairments, and executive function deficits in individuals with KS, comprehensive research on the neuropsychological profiles of affected children and adolescents remains limited. Additionally, KS has been associated with comorbid conditions such as depression, anxiety, schizophrenia, attention-deficit hyperactivity disorder (ADHD), and autism spectrum disorders (ASDs). However, systematic investigations into the neuropsychological manifestations of KS in pediatric populations are scarce. Therefore, the primary objectives of this review are to provide an overview of key studies examining the neuropsychological profiles of children and adolescents with KS and to delineate the limitations and implications of existing research findings. By synthesizing available literature, this review aims to bridge the gap in understanding the cognitive and behavioral characteristics of children and adolescents with KS, shedding light on potential avenues for future research and clinical interventions. Ultimately, this review serves as a valuable resource for clinicians, researchers, policymakers, parents, and educators involved in the assessment and management of the neuropsychological aspects of Klinefelter syndrome in pediatric populations.
Full article
(This article belongs to the Special Issue Mental Health and Psychiatric Disorders of Children and Adolescents)
►▼
Show Figures

Figure 1
Open AccessArticle
Radiographic and Tomographic Study of the Cranial Bones in Children with the Idiopathic Type of West Syndrome
by
Ali Al Kaissi, Sergey Ryabykh, Farid Ben Chehida, Hamza Al Kaissi, Vasileios Dougales, Vladimir M. Kenis and Franz Grill
Pediatr. Rep. 2024, 16(2), 410-419; https://doi.org/10.3390/pediatric16020035 - 24 May 2024
Abstract
►▼
Show Figures
Background: Neither radiological phenotypic characteristics nor reconstruction CT scan has been used to study the early anatomical disruption of the cranial bone in children with the so-called idiopathic type of West syndrome. Material and Methods: The basic diagnostic measures and the classical antiepileptic
[...] Read more.
Background: Neither radiological phenotypic characteristics nor reconstruction CT scan has been used to study the early anatomical disruption of the cranial bone in children with the so-called idiopathic type of West syndrome. Material and Methods: The basic diagnostic measures and the classical antiepileptic treatments were applied to these children in accordance with the conventional protocol of investigations and treatment for children with West syndrome. Boys from three unrelated families were given the diagnosis of the idiopathic type of West syndrome, aged 7, 10 and 12 years old. Parents underwent extensive clinical examinations. Three parents (age range of 28–41 year) were included in this study. All children showed a history of intellectual disabilities, cryptogenic epileptic spasms and fragmented hypsarrhythmia. These children and their parents were referred to our orthopedic departments because of variable skeletal deformities. Variable forms of skeletal deformities were the motive for the families to seek orthopedic advice. A constellation of flat foot, torticollis and early-onset osteoarthritis were observed by the family doctor. Apparently, and from the first clinical session in our practice, we felt that all these children are manifesting variable forms of abnormal craniofacial contour. Thereby, we immediately performed detailed cranial radiological phenotypic characterization of every affected child, as well as the siblings and parents, and all were enrolled in this study. All affected children underwent whole-exome sequence analysis. Results: The craniofacial phenotype of all children revealed apparent developmental anatomical disruption of the cranial bones. Palpation of the skull bones showed unusual palpable bony ridges along different sutural locations. A 7-year-old child showed abnormal bulging over the sagittal suture, associated with bilateral bony ridges over the squamosal sutures. AP skull radiograph of a 7-year-old boy with West syndrome showed facial asymmetry with early closure of the metopic suture, and other sutures seemed ill-defined. A 3D reconstruction CT scan of the skull showed early closure of the metopic suture. Another 3D reconstruction CT scan of the skull while the patient was in flexion showed early closure of the squamosal sutures, pressing the brain contents upward, causing the development of a prominent bulge at the top of the mid-sagittal suture. A reformatted 3D reconstruction CT scan confirmed the bilateral closure of the squamosal suture. Examination of the parents revealed a similar skull radiographic abnormality in his mother. A 3D reformatted frontal cranial CT of a 35-year-old mother showed early closure of the metopic and sagittal sutures, causing a mid-sagittal bony bulge. A 10-year-old boy showed an extremely narrow frontal area, facial asymmetry and a well palpable ridge over the lambdoid sutures. A 3D axial reconstruction CT scan of a 10-year-old boy with West syndrome illustrated the asymmetry of the posterior cranial bones along the lambdoid sutures. Interestingly, his 28-year-old mother has been a client at the department of spine surgery since she was 14 years old. A 3D reconstruction CT scan of the mother showed a noticeable bony ridge extending from the metopic suture upwards to involve the sagittal suture (red arrow heads). The black arrow shows a well demarcated bony ridge over the squamosal suture. A 3D reconstruction CT scan of the skull and spine showed the thick bony ridge of the metopic and the anterior sagittal as well as bilateral involvement of the squamosal, causing apparent anterior narrowing of the craniofacial contour. Note the lumbar scoliosis. A 12-year-old boy showed brachycephaly. A lateral skull radiograph of a 12-year-old boy with West syndrome showed premature sutural fusion, begetting an abnormal growth pattern, resulting in cranial deformity. The nature of the deformity depends on which sutures are involved, the time of onset and the sequence in which individual sutures fuse. In this child, brachycephalic secondary to craniosynostosis, which occurred because of bilateral early ossification of the coronal sutures, led to bi-coronal craniosynostosis. Thickened frontal bones and an ossified interclinoid ligament of the sella turcica were encountered. The lateral skull radiograph of a 38-year-old mother with a history of poor schooling achievements showed a very similar cranial contour of brachycephaly, thickening of the frontal bones and massive ossification of the clinoid ligament of the sella turcica. Maternal history revealed a history of multiple spontaneous miscarriages in the first trimester of more than five times. Investigating his parents revealed a brachycephalic mother with borderline intelligence. We affirm that the pattern of inheritance in the three boys was compatible with the X-linked recessive pattern of inheritance. Whole-exome sequencing showed non-definite phenotype/genotype correlation. Conclusions: The aim of this study was sixfold: firstly, to refute the common usage of the term idiopathic; secondly, we feel that it could be possible that West syndrome is a symptom complex rather than a separate diagnostic entity; thirdly, to further detect the genetic carrier, we explored the connection between the cranial bones in children with West syndrome with what has been clinically observed in their parents; fourthly, the early life anatomical disruptions of the cranial bones among these children seem to be heterogeneous; fifthly, it shows that the progressive deceleration in the development of this group of children is highly connected to the progressive closure of the cranial sutures; sixthly, we affirm that our findings are novel.
Full article

Figure 1
Open AccessArticle
Impact of the Omicron Strain on Febrile Convulsions Requiring Hospitalization in Children: A Single-Center Observational Study
by
Masayuki Nagasawa, Teruyoshi Shimoyama, Sayuri Hashimoto, Ryuichi Nakagawa, Haruna Yokoyama, Mari Okada, Tomohiro Udagawa and Akihiro Oshiba
Pediatr. Rep. 2024, 16(2), 399-409; https://doi.org/10.3390/pediatric16020034 - 14 May 2024
Abstract
►▼
Show Figures
Background. The emergence of the Omicron strain of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) at the end of December 2021 has drastically increased the number of infected children in Japan, along with the number of children with febrile convulsions, but its clinical
[...] Read more.
Background. The emergence of the Omicron strain of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) at the end of December 2021 has drastically increased the number of infected children in Japan, along with the number of children with febrile convulsions, but its clinical impact is unclear. Materials and Methods. We compared the frequency of SARS-CoV-2 infection in children hospitalized with febrile convulsions with the frequency of SARS-CoV-2 infection in children with fever and respiratory symptoms without convulsions. Results. In 2021 and 2022, 49 and 58 children required emergency hospitalization for febrile convulsions (FC group) with status epilepticus or cluster spasms, in which 24 and 38 children underwent a Filmarray® respiratory panel test (FA test), respectively, and others received a quantitative antigen test for SARS-CoV-2. In 2022, only six patients tested positive for SARS-CoV-2 (10.3%, 6/58). As a reference group, 655 children aged <10 years who underwent the FA test for fever and respiratory symptoms during the same period were investigated, and 4 (1.8%, 4/223) and 42 (9.7%, 42/432) tested positive for SARS-CoV-2 in 2021 and 2022, respectively. Rhinovirus/enterovirus (RV/EV) was the most frequently detected virus (40.3%, 264/655), followed by respiratory syncytial virus (RSV) (18.9%, 124/655) and parainfluenza virus 3 (PIV3) (7.8%, 51/655). There was no significant difference in the trend of detected viruses between the two groups. Conclusions. The frequency and severity of febrile convulsions requiring hospitalization associated with SARS-CoV-2 infection of the Omicron strain may be similar to that of other respiratory viruses in children.
Full article

Figure 1
Open AccessReview
Preservation of Pancreatic Function Should Not Be Disregarded When Performing Pancreatectomies for Pancreatoblastoma in Children
by
Traian Dumitrascu
Pediatr. Rep. 2024, 16(2), 385-398; https://doi.org/10.3390/pediatric16020033 - 13 May 2024
Abstract
►▼
Show Figures
Complete surgical resection in the context of a multimodal approach has been associated with excellent long-term survival in children diagnosed with pancreatoblastoma (PB). Traditionally, curative intent surgery for PB implies standard pancreatic resections such as pancreaticoduodenectomies and distal pancreatectomies with splenectomies, surgical procedures
[...] Read more.
Complete surgical resection in the context of a multimodal approach has been associated with excellent long-term survival in children diagnosed with pancreatoblastoma (PB). Traditionally, curative intent surgery for PB implies standard pancreatic resections such as pancreaticoduodenectomies and distal pancreatectomies with splenectomies, surgical procedures that may lead to significant long-term pancreatic functional deficiencies. Postoperative pancreatic functional deficiencies are particularly interesting to children because they may interfere with their development, considering their long life expectancy and the significant role of pancreatic functions in their nutritional status and growth. Thus, organ-sparing pancreatectomies, such as spleen-preserving distal pancreatectomies and central pancreatectomies, are emerging in specific tumoral pathologies in children. However, data about organ-sparing pancreatectomies’ potential role in curative-intent PB surgery in children are scarce. Based on the literature data, the current review aims to present the early and late outcomes of pancreatectomies in children (including long-term deficiencies and their potential impact on the development and quality of life), particularly for PB, and further explore the potential role of organ-sparing pancreatectomies for PB. Organ-sparing pancreatectomies are associated with better long-term pancreatic functional outcomes, particularly central pancreatectomies, and have a reduced impact on children’s development and quality of life without jeopardizing their oncological safety. The long-term preservation of pancreatic functions should not be disregarded when performing pancreatectomies for PB in children. A subset of patients with PB might benefit from organ-sparing pancreatectomies, particularly from central pancreatectomies, with the same oncological results as standard pancreatectomies but with significantly less impact on long-term functional outcomes.
Full article

Figure 1
Open AccessArticle
Association between Paediatric Complementary and Alternative Medicine Use and Parental Health Literacy, Child Health, and Socio-Economic Variables: A Prospective Study
by
Abida Denny, Andrew S. Day and Angharad Vernon-Roberts
Pediatr. Rep. 2024, 16(2), 368-384; https://doi.org/10.3390/pediatric16020032 - 8 May 2024
Abstract
►▼
Show Figures
Complementary and Alternative Medicines (CAMs) constitute products and practices not considered allopathic medicine. CAM use is high in children, but little is known about factors that may influence parents using CAM with their child. This study aimed to determine the variables associated with
[...] Read more.
Complementary and Alternative Medicines (CAMs) constitute products and practices not considered allopathic medicine. CAM use is high in children, but little is known about factors that may influence parents using CAM with their child. This study aimed to determine the variables associated with CAM use in children with a prospective study among children and their parents attending a tertiary care hospital in New Zealand (NZ). Outcomes included current CAM use, parental opinions on CAM, parental health literacy and child well-being. This study was completed by 130 parents (85% female), and the mean child age was 6.7 years. CAM use was reported for 59 (45%) children, the most common being oral supplements and body manipulation. Children were more likely to use CAM if their parent had higher health literacy (p = 0.001), and if they had previously attended the emergency department within 12 months (p = 0.03). There was no association between child well-being and CAM use. Parental opinion of using CAM only if a doctor recommended it was associated with CAM use for their child (p = 0.01). Only 40% of parents disclosed their child’s CAM use to the medical team. This study highlights that parental health literacy influences the use of CAM for children in NZ, providing insight for translational research to improve CAM safety and disclosure rates in NZ.
Full article

Figure 1
Open AccessBrief Report
Adolescents Identify Modifiable Community-Level Barriers to Accessing Mental Health and Addiction Services in a Rural Canadian Town: A Survey Study
by
Hana Marmura, Regina R. F. Cozzi, Heather Blackburn and Oliva Ortiz-Alvarez
Pediatr. Rep. 2024, 16(2), 353-367; https://doi.org/10.3390/pediatric16020031 - 6 May 2024
Abstract
►▼
Show Figures
Adolescents are particularly vulnerable to inadequate provision of mental health and addictions care, as services have been traditionally conceptualized to serve the needs of children or adults. Additionally, rural communities have been largely excluded from research investigating mental healthcare access and exhibit unique
[...] Read more.
Adolescents are particularly vulnerable to inadequate provision of mental health and addictions care, as services have been traditionally conceptualized to serve the needs of children or adults. Additionally, rural communities have been largely excluded from research investigating mental healthcare access and exhibit unique barriers that warrant targeted interventions. Finally, perspectives from the target population will be most important when understanding how to optimize adolescent mental health and addictions care. Therefore, the purpose of this study was to identify what adolescents in a rural town perceive as barriers to accessing mental health services. We conducted a cross-sectional survey study with high school students to generate ranked lists of the top perceived individual-level, community-level, and overall barriers. A total of 243 high school students responded to the survey. Perceived barriers were predominantly at the community level. Overall, the top barriers reported were a lack of awareness and education regarding mental health, resources, and the nature of treatment. Students who had previously accessed mental health services identified primary barriers related to mental health professionals, whereas students who had not accessed care reported fear and uncertainty as primary barriers. Modifiable community-level factors related to (1) mental health literacy and (2) mental healthcare professionals were identified by adolescents as the main perceived barriers to accessing mental health and addiction services in a rural town. The findings of this preliminary study should inform intervention strategies and further rigorous research for this traditionally underserved target population.
Full article

Figure 1
Open AccessArticle
Early Postnatal Administration of Erythropoietin and Its Association with Neurodevelopmental Outcomes and Incidence of Intraventricular Hemorrhage and Hypoxic-Ischemic Encephalopathy: A Four-Week Observational Study
by
Oana Cristina Costescu, Aniko Maria Manea, Eugen Radu Boia, Daniela Mariana Cioboata, Florina Marinela Doandes, Ileana Enatescu, Sergiu Costescu, Mihaela Prodan and Marioara Boia
Pediatr. Rep. 2024, 16(2), 339-352; https://doi.org/10.3390/pediatric16020030 - 28 Apr 2024
Abstract
►▼
Show Figures
This study aimed to investigate the impact of early erythropoietin (EPO) administration on the neurodevelopment of newborns, specifically focusing on its effects on hypoxic-ischemic encephalopathy (HIE) and intraventricular hemorrhage (IVH). The primary objective was to determine whether early EPO administration could impact the
[...] Read more.
This study aimed to investigate the impact of early erythropoietin (EPO) administration on the neurodevelopment of newborns, specifically focusing on its effects on hypoxic-ischemic encephalopathy (HIE) and intraventricular hemorrhage (IVH). The primary objective was to determine whether early EPO administration could impact the short-term neurodevelopmental outcomes and provide safety in neonates at risk for neurodevelopmental disorders. Conducted at the “Louis Turcanu” Children’s Emergency Clinical Hospital in Timisoara, Romania, this observational study included 121 neonates receiving EPO and 130 No EPO controls. EPO was administered within the first 48 h of life, with doses of 1000 U/kg that escalated to 2000 U/kg if necessary. Besides observing the occurrence of IVH and HIE, this study measured clinical and biochemical markers, including LDH, blood glucose, urea, creatinine, CPK, CRP, PCT, and erythropoietin levels alongside hematology and coagulation profiles. There were no significant differences in baseline characteristics between the groups. The EPO group showed significant reductions in LDH levels from days 1–3 to 7–10 (695.0 U/L to 442.0 U/L) and the APTT value (54.0 s) compared with the No EPO group (38.0 s). Notably, early EPO administration was associated with a significant decrease in HIE severity (beta coefficient: −0.38, p = 0.001). Additionally, lower gestational ages and hemoglobin levels correlated with increased severity of HIE. By week four, there was a significant reduction in moderate and severe HIE cases in the EPO group compared with controls (p = 0.001). Early administration of EPO in neonates significantly reduced the severity of IVH and HIE, suggesting its potential as a neuroprotective agent in neonatal care.
Full article

Figure 1
Open AccessReview
Assisted Reproductive Technologies: A New Player in the Foetal Programming of Childhood and Adult Diseases?
by
Gavino Faa, Mirko Manchia and Vassilios Fanos
Pediatr. Rep. 2024, 16(2), 329-338; https://doi.org/10.3390/pediatric16020029 - 26 Apr 2024
Abstract
Assisted reproductive technology (ART) is an emerging field in medicine that incorporates complex procedures and has profound ethical, moral, social, religious, and economic implications not just for the individuals who have access to this method but also for society. In this narrative review,
[...] Read more.
Assisted reproductive technology (ART) is an emerging field in medicine that incorporates complex procedures and has profound ethical, moral, social, religious, and economic implications not just for the individuals who have access to this method but also for society. In this narrative review, we summarise multiple aspects of ART procedures and the possible consequences on the mother and newborn. Moreover, we provide an overview of the possible long-term consequences of ART procedures on the health of newborns, although longitudinal evidence is particularly scant. Users should be informed that ART procedures are not risk-free to prepare them for the possible negative outcomes that may occur in the perinatal period or even in childhood and adulthood. Indeed, risk estimates point to increased liability for major nonchromosomal birth defects; cardiovascular, musculoskeletal, and urogenital (in male newborns) defects; and any other birth defects. Less certainty is present for the risk of neuropsychiatric sequelae in children conceived through ART. Thus, its application should be accompanied by adequate counselling and psychological support, possibly integrated into specific multidisciplinary clinical programmes.
Full article
(This article belongs to the Section Inborn Errors and Neonatal Screening)
Open AccessEditorial
The Burden of Not Doing
by
Maurizio Aricò
Pediatr. Rep. 2024, 16(2), 327-328; https://doi.org/10.3390/pediatric16020028 - 25 Apr 2024
Abstract
The cultural and professional growth of a physician is a long process, spanning over more than 10 years [...]
Full article
Open AccessArticle
Predictive Value of Neutrophil-to-Monocyte Ratio, Lymphocyte-to-Monocyte Ratio, C-Reactive Protein, Procalcitonin, and Tumor Necrosis Factor Alpha for Neurological Complications in Mechanically Ventilated Neonates Born after 35 Weeks of Gestation
by
Daniela Mariana Cioboata, Marioara Boia, Aniko Maria Manea, Oana Cristina Costescu, Sergiu Costescu, Florina Marinela Doandes, Zoran Laurentiu Popa and Dorel Sandesc
Pediatr. Rep. 2024, 16(2), 313-326; https://doi.org/10.3390/pediatric16020027 - 24 Apr 2024
Abstract
►▼
Show Figures
This prospective study investigated the association between elevated neutrophil-to-monocyte ratio (NMR), lymphocyte-to-monocyte ratio (LMR), C-reactive protein (CRP), procalcitonin, and tumor necrosis factor-alpha (TNF-alpha) and the risk of develo** neurological complications in mechanically ventilated neonates. The aim was to evaluate these biomarkers’ predictive value
[...] Read more.
This prospective study investigated the association between elevated neutrophil-to-monocyte ratio (NMR), lymphocyte-to-monocyte ratio (LMR), C-reactive protein (CRP), procalcitonin, and tumor necrosis factor-alpha (TNF-alpha) and the risk of develo** neurological complications in mechanically ventilated neonates. The aim was to evaluate these biomarkers’ predictive value for neurological complications. Within a one-year period from January to December 2022, this research encompassed neonates born at ≥35 weeks of gestational age who required mechanical ventilation in the neonatal intensive care unit (NICU) from the first day of life. Biomarkers were measured within the first 24 h and at 72 h. Sensitivity, specificity, and area under the curve (AUC) values were calculated for each biomarker to establish the best cutoff values for predicting neurological complications. The final analysis included a total of 85 newborns, of which 26 developed neurological complications and 59 without such complications. Among the studied biomarkers, TNF-alpha at >12.8 pg/mL in the first 24 h demonstrated the highest predictive value for neurological complications, with a sensitivity of 82%, specificity of 69%, and the highest AUC (0.574, p = 0.005). At 72 h, TNF-alpha levels greater than 14.3 pg/mL showed further increased predictive accuracy (sensitivity of 87%, specificity of 72%, AUC of 0.593, p < 0.001). The NMR also emerged as a significant predictor, with a cutoff value of >5.3 yielding a sensitivity of 78% and specificity of 67% (AUC of 0.562, p = 0.029) at 24 h, and a cutoff of >6.1 showing a sensitivity of 76% and specificity of 68% (AUC of 0.567, p = 0.025) at 72 h. Conversely, CRP and procalcitonin showed limited predictive value at both time points. This study identifies TNF-alpha and NMR as robust early predictors of neurological complications in mechanically ventilated neonates, underscoring their potential utility in guiding early intervention strategies. These findings highlight the importance of incorporating specific biomarker monitoring in the clinical management of at-risk neonates to mitigate the incidence of neurological complications.
Full article
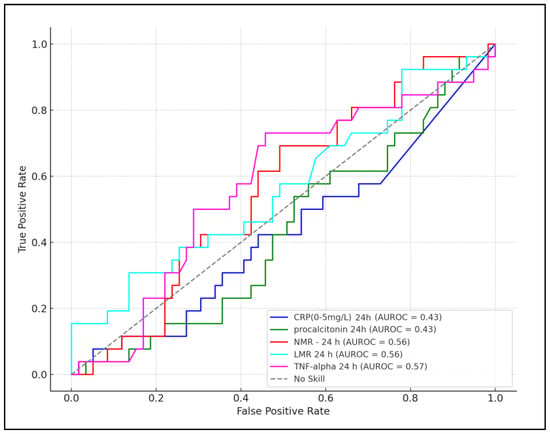
Figure 1
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics

Conferences
Special Issues
Special Issue in
Pediatric Reports
Global Neonatal Screening: Expanding Horizons in Diagnostic Technologies
Guest Editor: Victoria KainDeadline: 10 September 2024
Special Issue in
Pediatric Reports
Modern Solutions for Diagnosis and Treatment Planning in Pediatric Dentistry and Orthodontics
Guest Editors: Antonino Lo Giudice, Rosalia Leonardi, Vincenzo RonsivalleDeadline: 31 January 2025
Special Issue in
Pediatric Reports
Mental Health and Psychiatric Disorders of Children and Adolescents
Guest Editor: Artemis K. TsitsikaDeadline: 30 April 2025
Special Issue in
Pediatric Reports
Pediatric Cancers Risk Factors and Prevention
Guest Editor: Paraskevi A FaraziDeadline: 16 June 2025
Topical Collections
Topical Collection in
Pediatric Reports
COVID-19: What Happens in Pediatric Research in the Era of Pandemic
Collection Editor: Maurizio Aricò